Osteopathy & osteoarthritis
Introduction
Osteoarthritis, OA, arthrosis, wear and tear, joint degeneration … Do these terms sound familiar? Have you ever had these mentioned to you when discussing your aches and pains? They all mean the same thing! It is just that the more ‘technical’ sounding terms seems to hit home a little harder. Osteoarthritis (OA) is a perfectly natural process that begins from an earlier age than you may think. Depending on factors such as an individual’s levels of activity, previous trauma, weight and general health, the process can start as early as 35-years old. However a person may not feel any effects until their 50s and/or 60s.
What is Osteoarthritis?
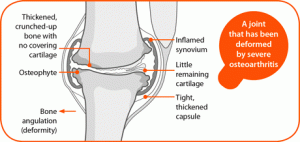
OA is a condition affecting joints, commonly the weight-bearing joints of the hips, knees and spine. It can also affect the fingers, thumbs, neck and big toes. The surfaces within the joints become damaged so that they don’t move as smoothly as they should. When a joint develops OA, some of the cartilage covering the ends of the bones gradually roughens and becomes thin, thickening the bone underneath. Tissues associated with the joint may then become more active than normal:
- The bone at the edge of the joint grows outwards, forming bony spurs called osteophytes;
- The inner layer of the joint capsule which produces fluid (synovium) may thicken and make extra fluid – causing the joint to swell;
- The capsule and ligaments slowly thicken and contract, in an attempt to repair or stabilise the joint.
OA should not be confused with the autoimmune condition Rheumatoid Arthritis (RA), where the body’s immune system (responsible for fighting infection) mistakenly attacks the cells lining the joints, making them swollen, stiff and painful. This can lead to early-onset OA due to joint disruption, but they are different conditions and separate in origin.
Symptoms
- Pain – often worse when the joint is moved or at the end of the day and felt more frequently with severe (advanced) OA;
- Stiffness – particularly after rest, usually eased by movement;
- Crepitus – a grating / grinding / creaking and/or crunching sensation from within the joint during movement;
- Swelling – possibly hard (caused by osteophytes) or soft (caused by synovial thickening and extra fluid) and the muscles around the joint may look thin and/or wasted;
- Restriction – joints may not move as freely or as far as normal, may sometimes give way because the muscles have weakened, or feel joint less stable.
Symptoms will often vary for no clear reason – with good and bad spells. Some people find that changes in the weather make their pain worse, especially damp and cold conditions. Others find that their pain varies depending on activity. Pain may disturb sleep and severe OA can disrupt daily movements.
Treatments
Osteopathy
Manipulation can help to improve the range of movement in osteoarthritic joints. It is not appropriate for everyone and Woburn Osteopaths will be able to advise whether it could be useful for specifically to you. Soft tissue massage and articulatory techniques are safe for almost all patients, helping to reduce muscle tension, maintain joint range of movement and ease pain.
Modern acupuncture
Modern acupuncture can sometimes help to ease OA-related pain and relax associated muscles. This can be useful in managing day to day pain of advanced OA, where manipulation and/or articulation techniques are too painful.
Strengthening exercises
Strengthening exercises will improve the strength and tone of the muscles controlling the joint, helping to protect / stabilise the joint and reduce pain. Keeping the supporting muscles of a joint strong can also provide a better outcome for joint replacement surgery.
Examples: http://www.arthritisresearchuk.org/arthritis-information/exercises-to-manage-pain.aspx
Weight loss
Being overweight puts extra strain on joints. If you are overweight, losing two stone (about 13 kg) can reduce the pain in an arthritic knee by up to 50%. Even a little weight loss can make a difference. A healthy, balanced, low-fat and nutritional diet with plenty of fruit, vegetables and fibre is optimal. Avoiding too much meat or animal fat is a good idea.
Pain control and NSAIDs
If you have pain caused by OA, your GP may suggest taking paracetamol at first. This is available over the counter in pharmacies without a prescription. Depending on the extent of joint degeneration, reducing the pain may enable joints to move and circulate the synovial fluid within them.
If paracetamol does not effectively control the pain, your GP may suggest or prescribe a non-steroidal anti-inflammatory drug (NSAID) such as ibuprofen or naproxen.
Surgery
Arthroscopy or ‘keyhole’ surgery can be used to help with diagnosis and/or may form part of treatment. Arthritic joints can be cleared of debris and effectively ‘tidied up’.
Surgery to replace the joint may be necessary if the joint damage is severe enough to continually disrupt everyday life and/or when other treatments have had minimal impact. Many different joints (e.g. hip, knee, shoulder and elbow) are routinely and successfully replaced in people with advanced OA.
Whilst there is no cure for the natural process of OA, a better understanding of it may help.
Woburn Osteopaths would be delighted to answer any OA-related questions: 01525 290615 / [email protected]
Useful links
http://www.arthritisresearchuk.org/
http://www.nhs.uk/conditions/Rheumatoid-arthritis/Pages/Introduction.aspx


